Migrants Are Scared to Get the Coronavirus Vaccine – and the Hostile Environment Is to Blame
by Sophie K Rosa
19 February 2021
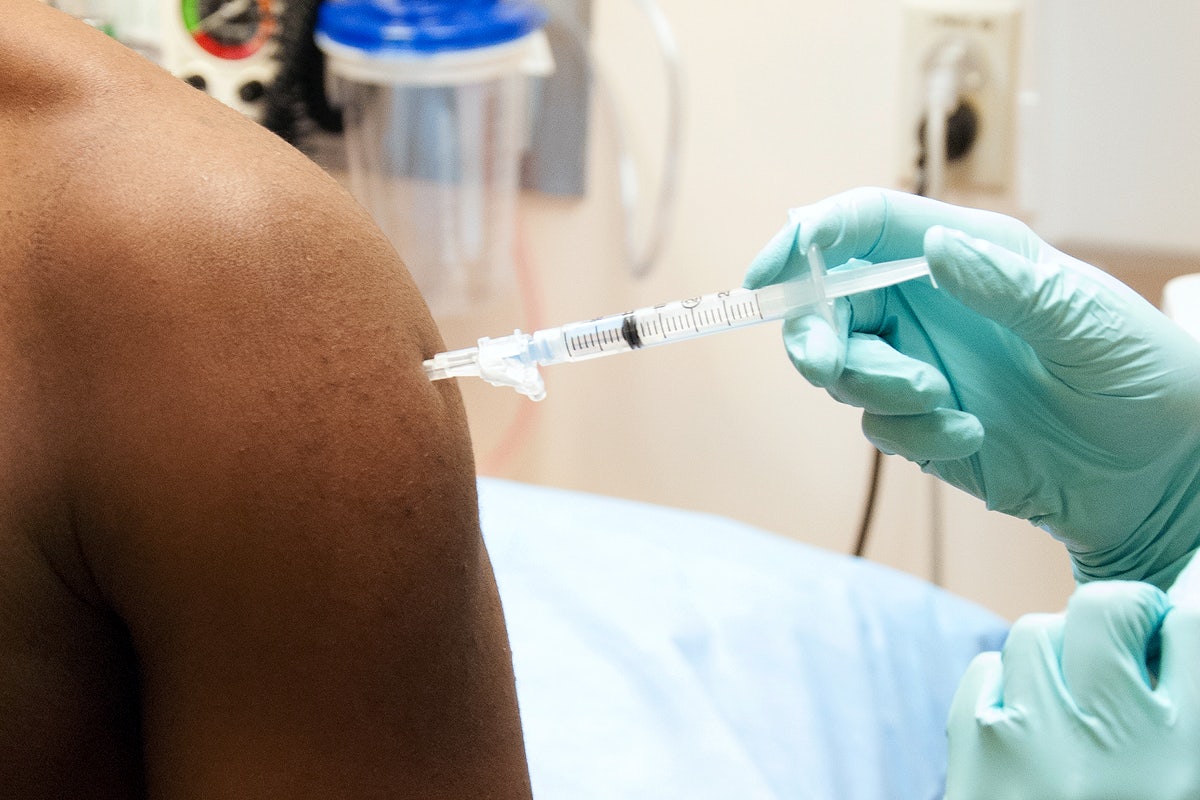
Since the government announced last week that “those who are here illegally can come forward to receive a vaccine,” Ali*, a Pakistani delivery driver in London, has been discussing the so-called amnesty with other migrants in a WhatsApp group. In the chat of more than 80 people – all of whom have precarious immigration status – Ali says that “everyone is scared to go and get the vaccine,” despite the government’s assurances.
These feelings reflect research published recently by the Joint Council for the Welfare of Immigrants (JCWI), which found that 43% of the migrants surveyed fear accessing healthcare during the coronavirus pandemic because of treatment charges or having their data shared with the Home Office – with data sharing being the predominant fear.
The report shows that the more precarious a migrant’s status, the more likely they are to be fearful. Eight out of ten migrants without any form of status said they are afraid to access healthcare, whilst 58% of those who have No Recourse to Public Funds, which does not prevent people from receiving NHS care, still reported being scared to do so. Even 17% of migrants with Indefinite Leave to Remain reported being scared to access healthcare, despite their status.
Our new @jcwi_uk report shows migrants are too afraid to seek healthcare, including (out of 310 surveyed):
▪️ 43% of all migrants
▪️ 56% of refugees
▪️ 58% of migrants with NRPF
➡️Findings in full: https://t.co/QOeX3QLg2K #VaccineForAll— JCWI (@JCWI_UK) February 9, 2021
But migrants and activists say the government’s announcement is nowhere near enough. “[It’s] hollow,” says James Skinner, a campaigner with Docs Not Cops, “you can’t give amnesty to a group of people who already have access to the thing you’re offering amnesty for.” He argues that, in itself, the government’s announcement reflects “a clear recognition… that the hostile environment is fundamentally incompatible with any kind of public health response.”
Everyone in the UK, regardless of their immigration status, is legally entitled to free primary healthcare (general practice, community pharmacy, dental and optometry services) – and in February 2020, the government added Covid-19 treatment to the list of treatments exempt from charges. Most secondary healthcare (specialist treatments), on the other hand, is chargeable – at up to 150% of the original cost – if a person is classed as a ‘temporary migrant’ or is undocumented. But despite the law, migrants face significant barriers to accessing the healthcare they are entitled to.
Joseph, a refugee from Zimbabwe, has experienced consistent gatekeeping when attempting to access healthcare. When he went to hospital with Covid-19 symptoms last year, he recalls being greeted by “a big sign outside that [said] folk have to prove they are entitled to use the NHS.” Once inside, he was asked by receptionists to prove his entitlement. “The government did change the law,” he says, “but the culture of checking has not changed.”
This lack of awareness among people working in healthcare, and in society more broadly, means that migrants often have to educate themselves and those around them about their rights, if they are to actually access the services they are entitled to. Joseph recalls how when he was undocumented, he was unable to register at a GP, despite being legally entitled to do so. Then, when he later gained asylum seeker status, he describes having to “teach a lot of healthcare professionals about [his] rights” in order to actually receive medical treatment.
But while Joseph, is well-versed in his rights as a migrant, a lot of migrants are not, meaning they avoid the healthcare system altogether for fear of repercussions. “There’s a huge problem with people being asked to provide ID or prove their entitlement to access [healthcare]… even though that’s actually not a requirement of registration,” explains Skinner. This creates “negative reinforcement” for migrants, who may come to associate healthcare with “requests for [documentation] you can’t provide, but also hostility from staff, who, for lots of reasons are overworked or under-resourced or don’t understand the very complex policies the government is trying to enforce.”
‘People are very, very sceptical – and quite rightly so.’
As a result of the way the hostile environment seeps into the healthcare system, Ali says that he, and most of the migrants he knows, believe that “if they take the vaccine… after a few months, [the Home Office will] get the data and [they will] be deported.”
Zoe Gardner, a policy adviser for JCWI, argues that this “climate of fear,” is related to a cultural “narrative of hostility” around migrants, “a narrative of ‘we’ll catch you out, we’ll send you back.’”
Many migrants also don’t trust that the medical attention will be free due to the complicated charging system. Garner cites the examples of both TB and HIV treatments for which migrants still sometimes face charges, despite being legally exempt for many years. “We have reams and reams of evidence and data that shows the fact that they’re exempt does not mean that all doctors and all administrative staff in the NHS know that they’re exempt, so people get wrongfully charged,” she explains. The very existence of a charging regime, she continues, creates an overall “deterrent effect” for migrants in need of healthcare.
Migrants’ fears around accessing healthcare, including the Covid-19 vaccination, are entrenched by wider systemic racism. Ali says he and many of his friends who are undocumented, or who have precarious immigration status, are cut off from vital sources of community and information. “They’re just doing work in hidden places, hidden factories,” he explains. “They don’t have circles [which could help them feel safe getting the vaccine].”
Joseph has been working hard to combat the spread of conspiracy theories about the vaccine. Doing so, however, has been difficult, given Britain’s racist past – and present. “Even if you can pretty much debunk the myths, for example, the myth that there is a chip [in the vaccine]…there is a lot of scepticism because folk are like, ‘You’ve treated us horribly for such a long time and then now all of a sudden there’s Covid-19 and you want to treat us so well. People are very, very sceptical – and quite rightly so.’”
Referencing historical medical racism as well as the violence currently happening in UK detention centres, Joseph argues that such examples are “just the tip of the iceberg” of what migrants in the UK endure. It is inevitable, he argues, that longstanding systemic racism has led to deep mistrust.
Hey @Charles_HRH & @SkyNews you can’t talk about vaccine ‘hesitancy’ without looking at root causes of mistrust.#HostileEnvironment policies like NHS charging & data-sharing are designed to sow fear & exclude people.
Time to call for #VaccinesForAll 👉https://t.co/UF7eRBvihy https://t.co/yA83CSSVMm
— Medact (@Medact) February 18, 2021
In a letter to the government’s scientific advisors SAGE late last week, the JCWI called for a suspension of all hostile environment policies and the implementation of a vaccination programme that is truly safe for everyone to access, regardless of immigration status. Implementing such a policy would mean ending NHS charging and a “firewall between the NHS and the Home Office.” The letter also urges the government to put public health first by allowing everyone to access the benefits system, thus enabling migrants to refuse dangerous working conditions.
Over 140 charities, local authorities, faith groups and medical groups – including JCWI and Docs Not Cops – have written to the government calling for “a much more systematic and structured approach to undoing some of the fear that has been generated through the hostile environment,” says Skinner.
As well as providing free healthcare and protecting patents’ data from immigration enforcement, this would mean “working with public health teams and local organisations, to fund a substantial public health campaign that directly addresses the fears that the hostile environment has created,” he continues.
Ending the Hostile Environment is the first step to ensure people can access the NHS.
That’s why 230 organisations have called for @DHSCgovuk to:
🚫Guarantee NO data shared w @ukhomeoffice
🏥End NHS charging
🗣Ensure everyone knows their right to healthcare
#VaccinesForAll— Migrants Organise (@migrantsorg) February 18, 2021
Gardner points to the EU Settled Status Scheme – which processes applications of EU citizens currently living in the UK to allow them to remain in the UK post-Brexit – as an example of how this could work. As a result of significant funding and research, the scheme has been able to reach “different vulnerable groups, people who may not be so digitally literate… to inform these communities and to also provide assistance in making the application.” But even so, it hasn’t reached everyone.
Considering how much money and resources went into rolling out the settled status campaign, Gardner is adamant that the government should be doing far more to ensure that all migrants are confident about accessing the vaccine safely. “[The vaccine] is supposed to protect us all,” she says. The fact that the government has thus far only released a press release stating an existing policy is, therefore, “simply nowhere near enough.”
To rebuild trust with migrant communities, Joseph wants to see the government “categorically” assure people that the Covid-19 vaccination will not entail any data sharing with the Home Office. He also suggests that “doctors [who are] basically acting as border agents [should] go out into communities and do community outreach.”
Meanwhile, Gardner says the key to ensuring migrants feel safe accessing healthcare is changing the culture of fear the hostile environment has created. “You’ve got to change [it],” she says. “You’ve got to have a culture where people feel safe and feel respected and [that] they have a right to services, which they do.”
“The government [needs to own] what they broke,” says Joseph. “They broke the trust [of the migrant community]. If you break something, you fix it.”
*Identifying details have been changed to protect anonymity.
Sophie K Rosa is a freelance journalist. In addition to Novara Media, she writes for the Guardian, VICE, Open Democracy, CNN, Al Jazeera and Buzzfeed.