Queer Elders Are Going Into Care – And Back Into the Closet
Activists who started Pride are fighting for a care system that honours queer people in later life.
by Sophie K Rosa
11 June 2021

It was fellow residents who informed Ted Brown about the abuse his partner Tim*, who has dementia, was being subjected to by staff at his care home.
They recalled to Brown how two staff members taunted Tim, saying, “Are you a gay man? Do you like gay men?” before dragging him into his room, upon which there was “some kind of commotion”. Shortly afterwards, Brown discovered bruises and what appeared to be a cigarette burn on Tim’s hand.
Other residents asked Brown “not to let the staff know that they were lesbian or gay” for fear of “suffering the same” abusive treatment. They also advised Brown “to be very careful” when making complaints, since “retaliatory abuse might occur”.
In response to the incident, the perpetrators “were suspended for a while,” says Brown. However, this punishment was short-lived and the workers ultimately ended up being “moved to another floor” in the same home – despite it denying that the treatment Tim received was homophobic. Now, as a result of these failings, Brown, a lifelong activist who helped organise the first-ever UK Pride, is waging a bigger fight by taking his local authority to court.
Ted Brown helped organise the first UK Gay Pride march in 1972 – featuring a mass ‘kiss-in’ that defied the law. He also battled intense racism. Listen to his moving life story
https://t.co/vqVyQOsNTa pic.twitter.com/z2SmB0cdzs
— BBC World Service (@bbcworldservice) June 3, 2021
Homophobic abuse in care homes is on the rise. Compassion in Care, a charity campaigning for an end to such treatment, received 50 reports of homophobic abuse in homes between 2017 and 2019 – and has received many more since, according to founder Eileen Chubb, a former care worker and whistleblower.
Among the 50 incidents, most were verbal abuse related to homophobic beliefs, with 19 of those related to the exclusion of partners from care decisions. Based on the calls her helpline receives, Chubb believes discrimination against LGBTQ+ people in care has “gotten worse” in recent years. Almost half of the reports Compassion in Care receives relate to queerphobic abuse in care homes – and its data is unique, since local authorities don’t record instances of such abuse separately.
Geoff Hardy, the co-founder of Safe Ageing No Discrimination (SAND), has seen many loved ones pass through the care system, many of whom are LGBTQ+. “In the best scenario,” he explains, care staff will be polite and respectful; “in the worst”, queer people will face a “lack of dignity and abuse”.
Though campaigners including Brown, Hardy and Chubb say the Care Quality Commission (CQC) is failing to improve care for queer people, the discrimination they experience in the system is detailed in one of the CQC’s own reports: “Although lesbian, gay, bisexual and transgender (LGBT) people experience a higher incidence of life-limiting illness, the experience of LGBT people at the end of life has often been overlooked.” In conducting its research, the CQC spoke to residents in care homes, who shared experiences of having their identities ignored, prejudice, exclusion and being forced to deny their sexuality in order to feel safer.
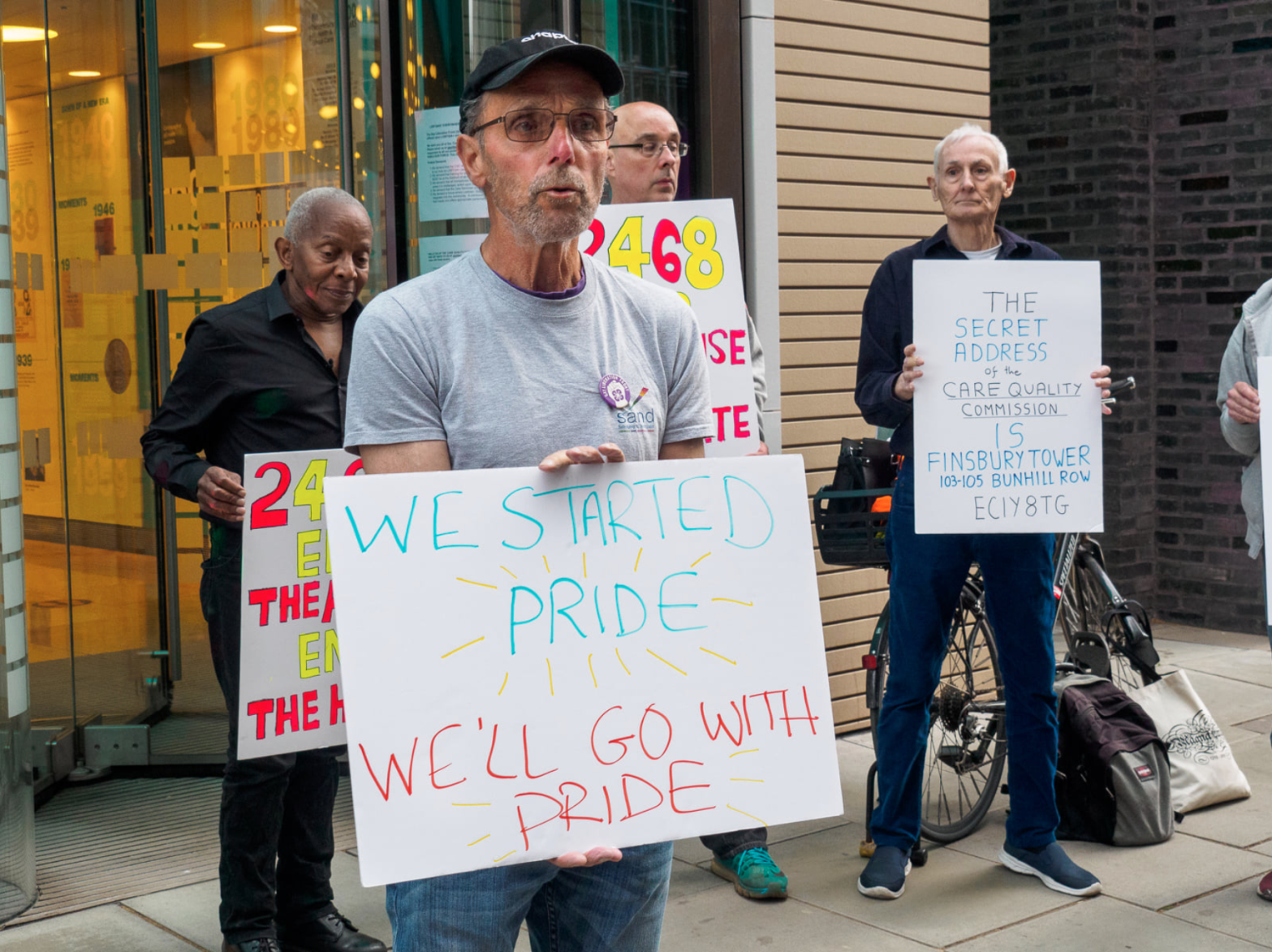
Older queer people are especially vulnerable to abuse when receiving care. “The person that abused them yesterday may be coming around to give them breakfast the next morning,” explains Brown. Experiencing prejudice can also be triggering, says Hardy, “Our past experiences of abuse, bullying, sidelining and the law… come back,” at a time in their life where people may be less able to resist.
Hardy points out that the majority of queerphobic abuse in care homes will not be reported since “to report abuse… you’ve actually got to come out [as gay].” In every case of homophobia reported to Compassion in Care, no or inadequate action was taken by the care home or the local authority. Chubb says that safeguarding processes are almost always ineffective, resulting in queer people being treated as “less than human”. Brown agrees that accountability is profoundly lacking in the system, adding that “disastrous” care homes often simply “change their names” instead of actually working to address their failings.
Heterosexism is often reflected in the treatment queer people experience in care. When Hardy’s close friend Jonathan Cutbill, the co-founder of Gay’s the Word bookshop in London, began receiving home care visits after a stroke, he was in the middle of curating “probably the finest LGBTQ+ library in Europe,” explains Hardy. However, having seen that the collection included photographs of gay men in “swimwear and skimpy clothing”, the care agency sent an unknown worker to Cutbill’s home, without any warning, in order to discipline him. “He was sleeping… and a voice came from above him,” recalls Hardy. The man – who failed to introduce himself – told Cutbill that he “shouldn’t have those images” visible in his home when staff were visiting. Subsequently, the agency refused to renew its contract with Cutbill. “There was absolutely no sense of Jonathan’s dignity,” says Hardy.
Thank you! It’s a joy to see & thanks to friends in Estates @UoLondon. Very fitting w/ @SenateHouseLib having one of the UK’s largest #LGBTQ collections inc. 30,000 items from Jonathan Cutbill, founder of @gaystheword & #LGBTrights activist 🏳️🌈 https://t.co/YL4cJsMOvE#PrideMonth
— Senate House Library (@SenateHouseLib) June 1, 2021
Discrimination against LGBTQ+ people receiving care often includes a failure to recognise non-heteronormative relationships, which can include preventing visits from partners. Although Tim’s care home was aware of his and Brown’s civil partnership (which they decided to get when Tim became unwell in order to access the legal authority to oversee his care), the staff persisted in miscategorising their relationship. On one occasion, Brown was referred to as Tim’s “son” – which Brown believes was intentional. On other occasions, Brown was excluded from important updates and decisions about Tim’s health and wellbeing.
The experiences of older LGBTQ+ people receiving care services are marked by heteronormative assumptions and aesthetics dominated by images of straight families, religious symbols and royal family memorabilia.
This heteronormativity in care may also take the form of insensitivity to queer people’s experiences in straight society. For example, older gay men are more likely to have married women and taken male lovers. If someone has dementia, explains Hardy, the person’s “other life” may come up in stories. But rather than honouring the person’s identity and sexuality in the present, their queerness will often be glossed over in favour of their more ‘palatable’ past. This kind of scenario is “abusive in the sense that it doesn’t recognise who you are,” says Hardy.
Christianity also often has a strong presence even in secular care homes. On Sundays, celebration days or at the end of someone’s life, priests often visit homes. Residents are often encouraged or even made to interact with them against their will, according to Hardy. For LGBTQ+ people who have experienced oppression related to religion, this can be a distressing experience – especially when they are encouraged to “repent their previous sinful lives”, says Brown.
Considering these risks, most queer people choose to ‘go back into the closet’ when receiving care services. Brown says that a lesbian woman he knows pretended that her partner of 20 years was a friend. Lately, he says he often wonders whether he and Tim would have been better off if they’d hidden their sexuality themselves.
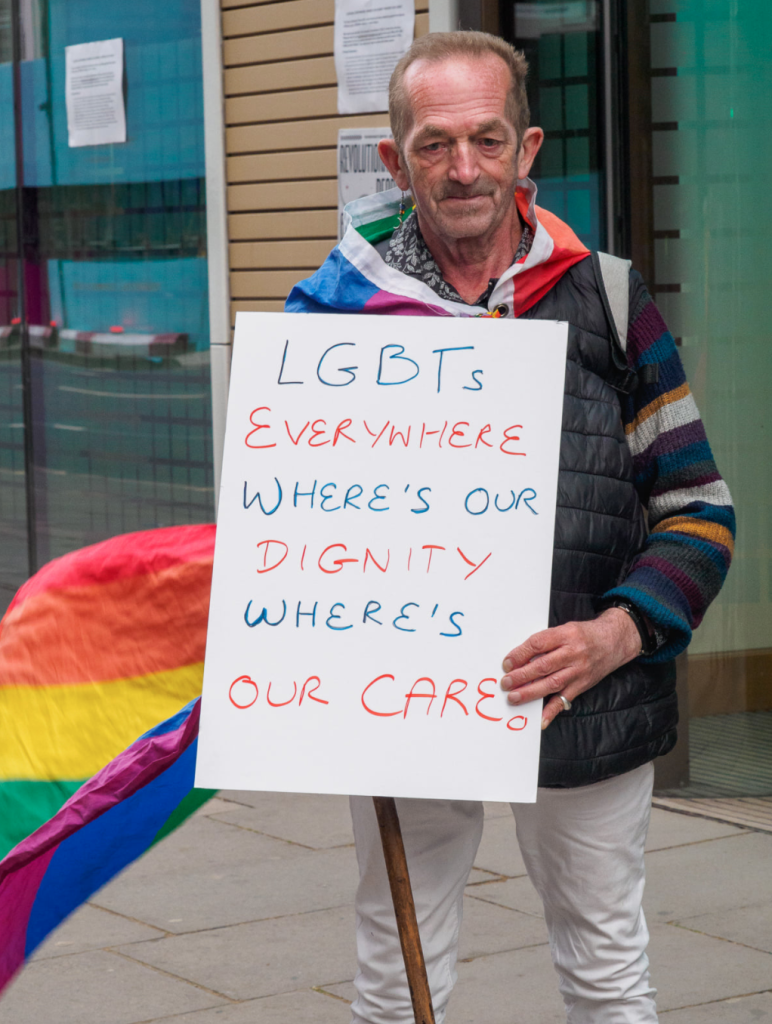
That said, the majority of care staff, of course, do not abuse the queer people in their care. “Most workers really do care,” says Hardy, “they may not understand things… but they’re not unkind.” As well as demanding a care system that is “fully responsive and accountable” to queer people, Hardy insists that part of improving the system – in which carers are overworked and underpaid – is ensuring that “everybody within it is valued and respected… that they are recompensed and recognised.”
Based on her own experience working in the system, Chubb believes that being a good care worker is having “the ability to make a person feel safe… and that they’ve got control and that their individuality is valued”. In terms of concrete policies that would make queer people in care safer, Chubb says that it is vital the system addresses homophobia and transphobia in the recruitment process, along with providing adequate training, protecting whistleblowers and acknowledging abuse by logging incidents by type.
As lifelong activists, Hardy and Brown are determined to keep fighting for queer liberation. “When you’re fighting for your own life, why would you give up?” asks Hardy. Both men admit to often overlooking the struggles of older queer people when they were young gay men. Now that he is 71, Hardy reflects that “in ten years, if I’m still here, I’ll be 81 and I want to be fully alive… to be recognised and valued.”
Last month, Brown and Hardy helped to organise a Gay Liberation Front protest outside of the Department of Health and Social Care, where they demanded a care system that recognises and respects the experiences and needs of queer people as they age.
After the homophobic abuse he received during his home care visits, Hardy’s friend Cutbill received visits from another agency – which, this time, reflected the kind of care campaigners are demanding. “The first thing [the new carer] did was ask him about who he was,” says Hardy, who used to attend the visits. Meanwhile, a mental health practitioner spent time celebrating the rich life Cutbill had led, asking him about his “amazing variety of books” and his diverse experiences. “What’s the most important thing? What really makes you feel that your life has been good?” Hardy recalls her asking. Cutbill told her that it was setting up his bookshop and creating his library. She expressed admiration for his work, commenting that he was a “pioneer”.
After this interaction, Hardy recalls how his friend “melted, he warmed, he started to open up… he started to share his life.” This is the kind of treatment all queer people deserve, says Hardy. “That is caring. That is applying dignity to somebody else.”
*Name has been changed.
If you would like to get involved with the campaign, email [email protected].
Sophie K Rosa is a freelance journalist. In addition to Novara Media, she writes for the Guardian, VICE, Open Democracy, CNN, Al Jazeera and Buzzfeed.