Ending Vaccine Apartheid Won’t End the Pandemic
We promised the Global South 2.1bn vaccines. Just 4% have been delivered.
by James Meadway
12 January 2022
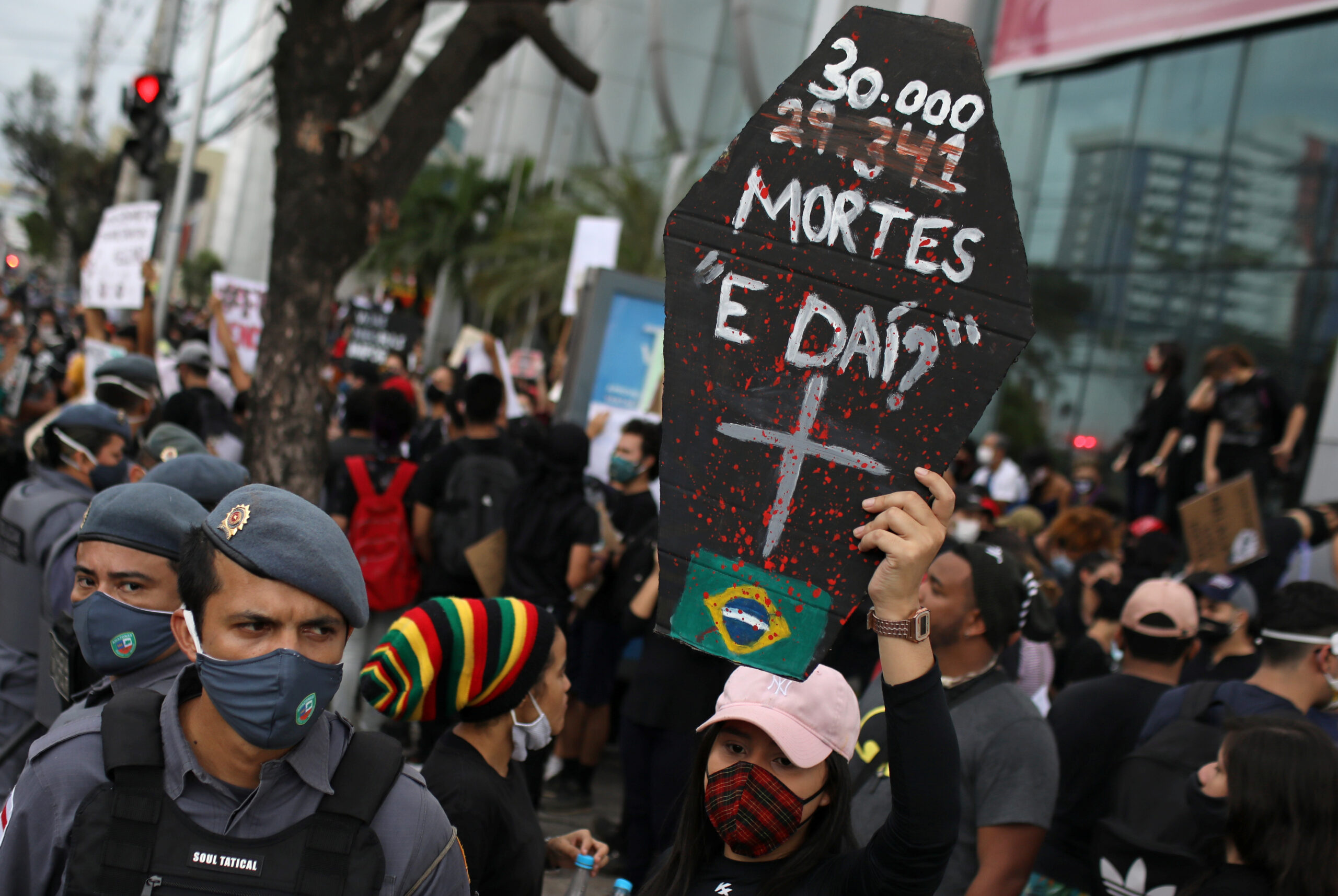
If we were actually serious about reducing the damage wrought by the coronavirus pandemic and limiting the prospect of future variants emerging, we should have rolled out a rapid and comprehensive global vaccination programme. Instead, rich countries in the global north quickly developed and distributed vaccines among their people, a vital resource they then refused to share with poorer countries in the global south – a decision that has contributed to millions of unnecessary deaths in the region.
Indeed, rather than bringing us closer to a conclusion to this rolling crisis, vaccines have added to the political chaos and dislocation of the pandemic.
Predictably, global capitalism is not capable of distributing an essential health service fairly and effectively – even if every major government and every international organisation agrees that this is what should happen. It is only pressure from below – from the movements for global health justice – that can force the system to act in the public interest.
What’s more, protecting society against coronavirus, and the new diseases we can expect in the future, will require a sophisticated programme of which mass vaccination campaigns are only one part.
Capitalism is the culprit.
Global vaccine inequality has become catastrophic over the course of the pandemic. On one side, rich countries in the global north have hoarded immense supplies of the available vaccines. Britain alone has ordered 650m doses – or more than ten for every citizen – and first-shot vaccination rates here have hit over 90%. Amongst high-income countries, the vaccination rate is now 77% and rising, with some rich countries already contemplating a fourth round of shots.
By contrast, low-income countries (where the average income is $1,045 a year or less) have suffered disastrously low vaccination rates, currently sitting at just over 8.8% of adults. By the end of last year, rich countries had distributed more booster shots than the total number of all vaccines administered in poorer countries.
Meanwhile, the World Health Organisation’s (WHO) Covax programme, which was set up with the intention of richer countries providing vast quantities of vaccines to poorer ones, has been a flop.
Vaccine Apartheid; a moral failure to enable equal access to tools to combat COVID
COVAX, has 600m doses for Africa; just a quarter of its 1.2bn population
$27bn is needed to fund vaccines for poorer nations; failure would cost lives, more mutations & the global economy $9.2tn
— Claudia Webbe MP (@ClaudiaWebbe) April 25, 2021
Just 4% of the 2.1bn vaccines promised by the developed world have been delivered. This failure to vaccinate populations has consequences for the whole world, rich and poor countries alike: large numbers of unvaccinated and uninfected people encourage the appearance of mutations in the virus. One plausible (but not the only) route for Omicron’s emergence is via an unvaccinated population.
The reasons for this failure are obvious. Capitalism is a competitive system, which pits company against company, nation against nation. The economic advantage for a government vaccinating its domestic population ahead of others is obvious, as Britain saw over the last year; the country’s economic growth was able to rebound rapidly as the vaccine rollout powered ahead.
The advantage in vaccinating globally, on the other hand, is much more diffuse: everyone would benefit, but there’s a good reason, in competitive, capitalist terms, not to bother paying for it yourself if everyone benefits.
Countries like China and Russia have attempted to use vaccine distribution in poorer countries as part of their diplomatic efforts to win favour – about half of all vaccines administered globally are from China.
This, however, is not enough to overcome the lack of effort from global north countries, and the outright opposition of pharmaceutical corporations to measures like patent waivers.
Some governments have encouraged an ugly turn against the unvaccinated, like that which we are seeing in France. President Macron recently said he would like to “emmerder” (roughly translated as ‘piss’ off) the unvaccinated, but generously offered to stop short of actually forcibly injecting people. More seriously, the Austrian government is moving to institute mandatory vaccines starting in February, and governments across the world – including those in the UK – have significantly restricted social life for those who are unvaccinated. Perhaps encouraged by these official signals, support for compulsion against the unvaccinated is currently high.
Vaccine prioritisation is key.
But rich countries hoarding vaccines and forcing them on the few remaining holdouts, whilst depriving millions of people access to them in poorer countries is not going to end the pandemic. Targeting the unvaccinated minority for abuse is useless, but provides a convenient scapegoat for the many failings of governments and corporations in the Global North.
The evidence is clear that serious illness and death from Covid-19 is directly linked to government spending cuts, low incomes, poor quality housing, and exposure to high-risk work. These are all longstanding social and economic problems, and are often linked to other kinds of discrimination, particularly on the grounds of race.
Imagine being asked to trust a govt that has consistently let down ethnic minority groups – with discriminatory policies (e.g. having to pay for the NHS twice for migrants), with a hostile environment (discriminatory immigration policies).
— Deepti Gurdasani (@dgurdasani1) May 18, 2021
The reasons for vaccine hesitancy are more complex but, similarly, the evidence shows that “white people who identify as English, Scottish, Welsh or British register vaccine uptake levels of more than 80%, whereas the current number for people from a Caribbean background is 52%; among those classified as Gypsy or Traveller, the figure is 28%.” It would be quite wrong to confuse this social problem with the relatively tiny minority of conspiracy theorists and outright fascists in the organised anti-vax movement.
Part of the problem with the scapegoating of the unvaccinated seems to have been the serious over-selling of vaccination in the early months of the roll-out – with governments and, sadly, some public health professionals encouraging people to see vaccination as the high-road out of the pandemic.
This no doubt encouraged take-up, but at the cost of long-term damage to the programme. As was suspected at the vaccine’s launch, but since confirmed in practice, the immunity we receive from the vaccines is impressively robust to begin with, but fades rather quickly. A programme of boosters is required to maintain immunity. Far from being a one-shot end to the pandemic, the most likely prospect currently is that we are committing to a rolling programme of vaccinations every three months or so, with no end in sight.
This prospect of a never-ending vaccination programme, potentially including the whole of humanity, has rightly provoked warnings about the need to target and prioritise vaccine resources. The WHO has been insisting that vaccinating the unvaccinated in poorer countries should take priority over delivering boosters in the richer – but to no avail.
The head of the UK’s Joint Committee on Vaccinations and Immunisation has warned that “we can’t vaccinate the planet every four to six months,” urging vaccine prioritisation instead of mass booster campaigns. Removing patent rights, squeezing out the profiteering of the pharmaceutical companies and making proper use of the pharmaceutical resources of the Global South would all help overcome some of those resource issues.
Vaccination is only part of the solution.
But there are likely to be future limits on how far any vaccination programme, even a perfectly coordinated global system, will take us. It’s worth bearing in mind that only one human disease has ever been eradicated; smallpox was declared officially extinct in the wild by the WHO in 1980, after the last reported case in nature in 1977. Vaccination made this possible.
This, however, took two centuries to achieve – from Edward Jenner’s first successful smallpox vaccine in 1757 to its eventual eradication in 1980. Polio has been targeted for eradication in the wild by the WHO since 1988, but, whilst cases have been hugely reduced through vaccination campaigns, it remains stubbornly hard to eliminate.
For Covid-19, a respiratory illness that is now in very wide circulation, the chances of eradication through vaccination are essentially zero. Throw in the spread of the SARS-Cov-2 virus to animal populations that live near us, which provides the conditions for the virus to mutate – one of which has been suggested as another probable source for the Omicron variant – and even managing the disease in the future is likely to prove a significant strain on healthcare systems and economies.
Waiving patents on vaccines, and thus allowing their production to take place at lower cost in the global south, is an essential first step, and has been called for by the People’s Vaccine Alliance, a coalition of campaigning organisations, trade unions, and political leaders in the Global South.
Health and social care systems, in Britain and across the world, need more funding to build in additional capacity for future coronavirus outbreaks, and taxing wealth is the fairest way to make that happen. We will also need more support not only for people to have sick pay and time off work, but for economies to be built more around allowing working from home, reduced working hours and limiting commuting in order to minimise future risks.
Globally, vaccinations will remain critical to the future management of the virus. The failure to vaccinate the world fully and effectively has been a decisive factor in prolonging the first, crisis phase of the pandemic. But vaccines are only one part of the programme we need to get on top of coronavirus, and blaming the unvaccinated for a systemic failure will not bring the end of the pandemic any closer.
James Meadway is an economist.


